
Ney Carter Borges: Ticagrelor vs Prasugrel After PCI in Patients With Diabetes and MCAD
Ney Carter Borges, Member Cardiologist of Global Physician Association at Cleveland Clinic Florida, shared a post on LinkedIn:
“Ticagrelor vs Prasugrel After PCI in Patients With Diabetes and Multivessel Coronary Artery Disease
Patients with diabetes mellitus undergoing percutaneous coronary intervention (PCI) represent a particularly high-risk population due to enhanced platelet reactivity, increased thrombotic burden, and a greater incidence of recurrent ischemic events.
Potent P2Y12 inhibitors are therefore recommended as part of dual antiplatelet therapy (DAPT) following PCI. A recent randomized multicenter study evaluated the comparative clinical outcomes of ticagrelor versus prasugrel in patients with diabetes and multivessel coronary artery disease undergoing PCI with drug-eluting stents.
The trial enrolled approximately 1,800 patients across multiple centers between 2020 and 2024. Participants had documented diabetes mellitus and angiographically confirmed multivessel coronary artery disease requiring PCI. Patients were randomized to receive either ticagrelor (90 mg twice daily) or prasugrel (10 mg once daily), both administered in combination with aspirin as standard DAPT.
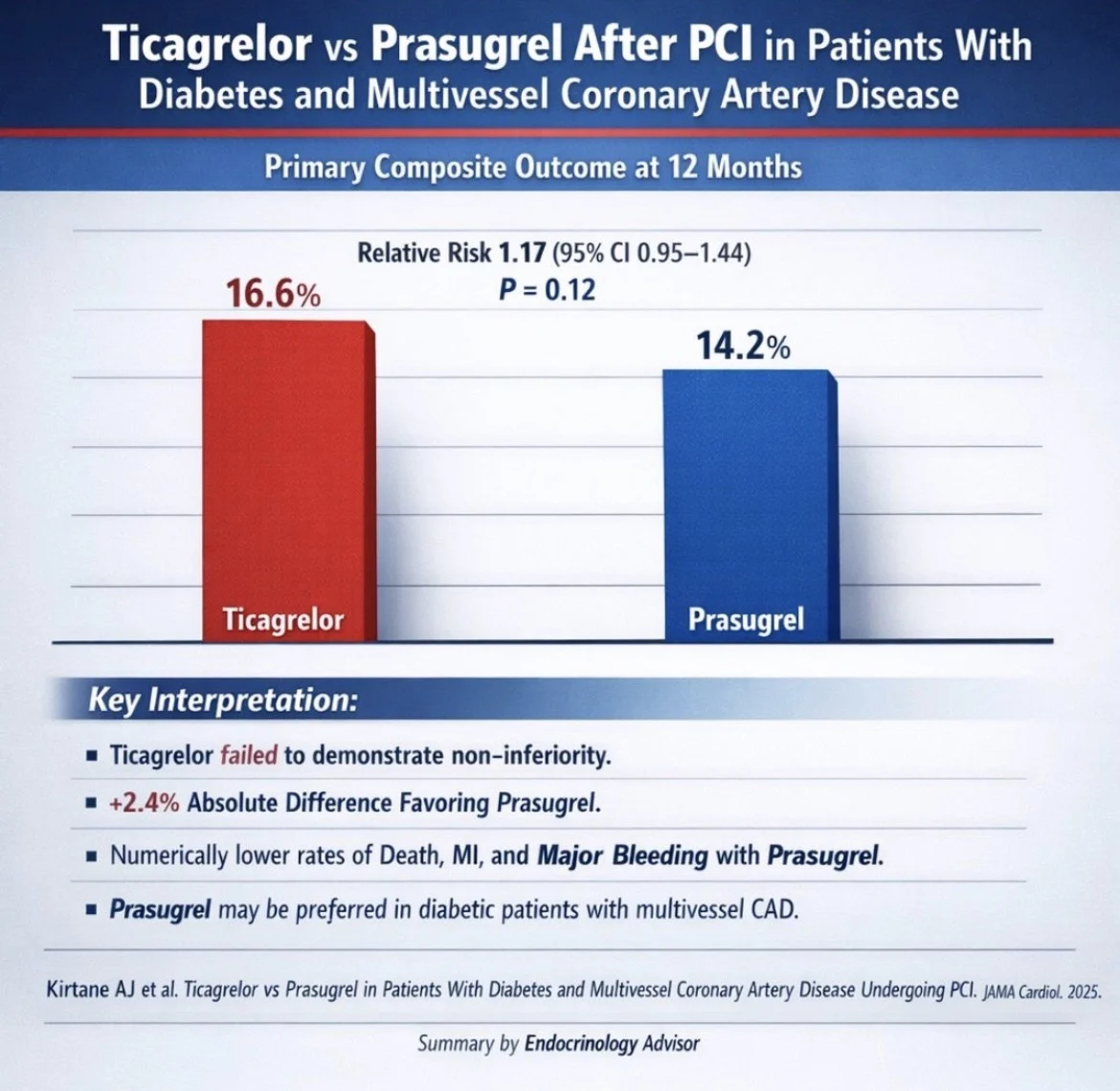
The primary endpoint was a composite of all-cause death, myocardial infarction, stroke, or major bleeding within 12 months after PCI. The composite endpoint occurred in 16.6% of patients treated with ticagrelor compared with 14.2% of those receiving prasugrel, corresponding to a relative risk of 1.17 (95% CI 0.95–1.44; p = 0.12).
Ticagrelor therefore failed to demonstrate non-inferiority compared with prasugrel. Individual clinical events, including death and myocardial infarction, were numerically lower in the prasugrel group, although differences were not statistically significant when analyzed separately.
These findings suggest that prasugrel may provide slightly more favorable outcomes in diabetic patients with complex coronary disease undergoing PCI. The results reinforce the concept that potent platelet inhibition strategies may not be fully interchangeable in high-risk populations. While both agents remain guideline-supported options for DAPT after PCI, this study highlights a potential clinical advantage of prasugrel in patients with diabetes and multivessel coronary artery disease.”
Other posts featuring Ney Carter Borges on Hemostasis Today.
-
May 12, 2026, 16:46Tagreed Alkaltham: Why Apheresis Matters in Modern Transfusion Medicine
-
May 12, 2026, 16:37Reinhold Kreutz: Cardiovascular Burden in Acute Intermittent Porphyria Needs Greater Awareness
-
May 12, 2026, 16:33Pablo Corral: The Truth About Very Low LDL-Cholesterol
-
May 12, 2026, 16:24Mildred Lundgren: We Must Talk About the Invisible Causes of Stroke
-
May 12, 2026, 16:17Irene Scala: The Sex Disparities In Access to Acute Stroke Treatments In Italy
-
May 12, 2026, 16:04May Nour: UCLA Health Mobile Stroke Unit Becomes The 1st In The World to Perform mCTA In the Field
-
May 12, 2026, 15:57Leonardo Roever: Prognostic Impact of Lipoprotein(a) and CAR in Elderly Acute Ischemic Stroke Patients
-
May 12, 2026, 15:54Bruno Pougault: Prioritizing Laboratory Tests in Resource-Limited Emergency Care
-
May 12, 2026, 15:37Jennifer Holter Chakrabarty: Supporting the Next Generation of Hematology Researchers

