
Ney Carter Borges: Endocrine Drivers of Resistant Hypertension – Insights from the MOMENTUM Trial at ACC 26
Ney Carter Borges, Member Cardiologist of Global Physician Association at Cleveland Clinic Florida, shared a post in LinkedIn:
“Endocrine Drivers of Resistant Hypertension: Insights from the MOMENTUM Trial / ACC 26
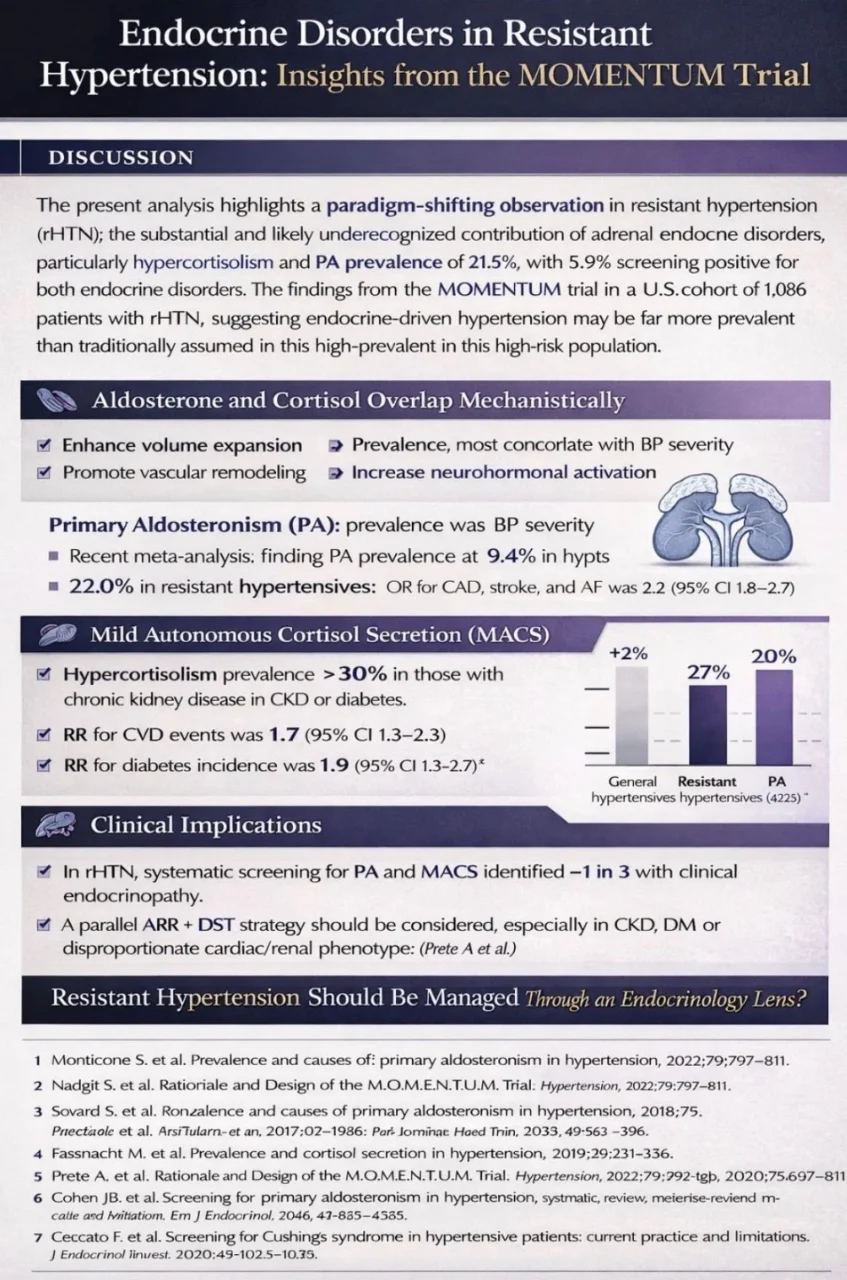
Resistant hypertension (rHTN) represents a high-risk clinical phenotype traditionally attributed to complex hemodynamic and pharmacologic factors. However, emerging evidence—highlighted by the MOMENTUM trial presented at ACC.26—suggests that underlying endocrine disorders, particularly hypercortisolism and primary aldosteronism (PA), may play a substantially larger role than previously recognized.
In the MOMENTUM cohort of 1,086 patients with rHTN, hypercortisolism was identified in 27.3% of individuals, while PA screening was positive in 21.5%. Notably, 5.9% of patients demonstrated biochemical evidence of both conditions. These findings reinforce the concept that endocrine-driven hypertension is not only prevalent but frequently overlapping, challenging the traditional view of isolated hormonal etiologies.
Primary aldosteronism has long been recognized as the most common form of secondary hypertension, with prevalence increasing alongside hypertension severity.
Beyond its effects on sodium retention and volume expansion, aldosterone contributes to vascular remodeling, myocardial fibrosis, and an increased risk of atrial fibrillation, stroke, and heart failure, independent of blood pressure levels. In parallel, mild autonomous cortisol secretion (MACS)—often clinically silent—has gained attention for its association with metabolic dysfunction, insulin resistance, and adverse cardiovascular outcomes.
Mechanistically, aldosterone and cortisol share converging pathways that exacerbate hypertension. Cortisol, particularly in states of chronic mild excess, can activate mineralocorticoid receptors through saturation of 11β-HSD2, thereby mimicking aldosterone-like effects.
This overlap may explain the observed co-secretion phenotype and the persistence of elevated blood pressure despite multidrug therapy.
Importantly, the MOMENTUM data suggest a higher prevalence of hypercortisolism in patients with chronic kidney disease, diabetes, and established cardiovascular disease, supporting a bidirectional relationship between endocrine dysregulation and cardiometabolic burden. These observations underscore the need for a broader diagnostic framework in rHTN.
Despite guideline recommendations, real-world screening for PA remains low, and evaluation for hypercortisolism is even less standardized.
The current evidence supports a dual-hormone screening strategy incorporating both aldosterone-renin ratio (ARR) and overnight dexamethasone suppression testing (DST), particularly in patients with resistant hypertension and high-risk phenotypes.
Although full peer-reviewed data from MOMENTUM are awaited, the consistency of these findings with prior literature strengthens their clinical relevance.
Collectively, these data raise a critical question: should resistant hypertension be routinely approached through an endocrinology lens?”
More posts featuring Ney Carter Borges on Hemostasis Today.
-
May 24, 2026, 17:48Flora Peyvandi: Crucial Role of Placental ADAMTS13 in Perinatal Survival
-
May 24, 2026, 17:13Mahtab Mashayekhi: The Evolving Role of Red Blood Cell Exchange in the Management of SCD
-
May 24, 2026, 17:12Silvina Graña: Helping Families Better Understand Hemophilia and Daily Life With Bleeding Disorders
-
May 24, 2026, 17:11Miikka Vikkula: Key Insights from the ISSVA 2026 World Congress
-
May 24, 2026, 17:10Mathieu Jackson: Proud to Be Present at This Historic Moment for the Global Bleeding Disorders Community
-
May 24, 2026, 17:09Ramina Fazeli: Highlighting the Emerging Role of Neutrophil Extracellular Traps in Ovarian Cancer
-
May 24, 2026, 16:12William Wallace: Normal B12 Levels May Still Cause Brain Damage and Cognitive Decline
-
May 24, 2026, 15:54Marc Carrier: Ottawa Race Weekend Raised Over 7,000 USD for Thrombosis Canada
-
May 24, 2026, 15:44Janak Sadhu: Building a Stroke-Free Mehsana Through Community Awareness and Healthcare Collaboration

