
Simon Senanu: Key Laboratory Markers of Hemolytic Anemia
Simon Senanu, Medical Laboratory Scientist at Perkins Medical Centre, shared a post on LinkedIn:
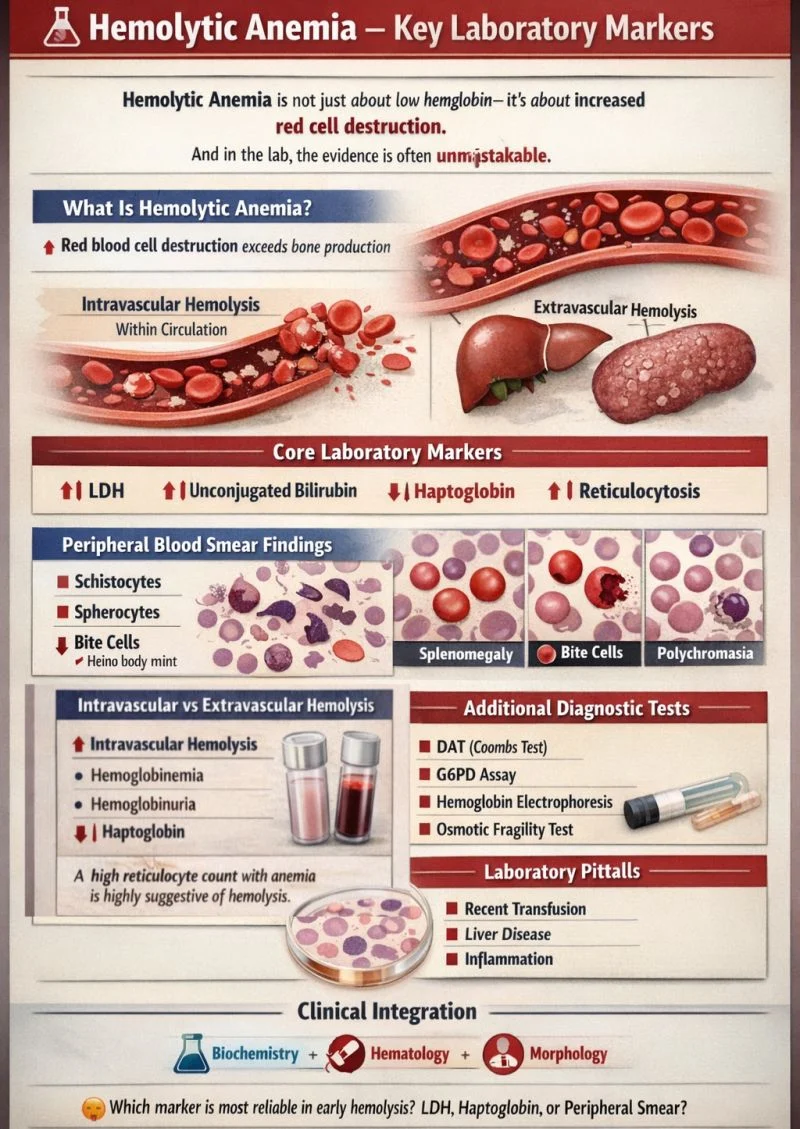
“Hemolytic Anemia – Key Laboratory Markers
Hemolytic anemia is not just about low hemoglobin – it’s about increased red cell destruction.
And in the lab, the evidence is often unmistakable.
What Is Hemolytic Anemia?
Hemolytic anemia occurs when:
- Red blood cell destruction exceeds bone marrow production
It can be broadly classified as:
- Intravascular hemolysis – destruction within the circulation
- Extravascular hemolysis – destruction by macrophages in the spleen and liver
- The distinction is critical, as it directly influences both laboratory findings and clinical presentation.
Core Laboratory Markers
The diagnosis relies on a combination of findings:
- Elevated Lactate Dehydrogenase (LDH) – Reflects cellular breakdown; often markedly increased in intravascular hemolysis
- Increased Unconjugated Bilirubin – Result of heme catabolism; may lead to clinical jaundice
- Reduced Haptoglobin – Binds free hemoglobin; levels drop as it is consumed – Often undetectable in intravascular hemolysis
- Reticulocytosis -Indicates marrow compensation, Reticulocyte count may rise within 3 – 5 days of hemolysis
A high reticulocyte count with anemia strongly suggests a hemolytic process.
Peripheral Blood Smear Findings
The blood film is indispensable in narrowing the cause:
- Schistocytes – Microangiopathic hemolytic anemia (e.g., TTP, DIC)
- Spherocytes – Autoimmune hemolytic anemia or hereditary spherocytosis
- Bite cells / Heinz body remnants – Oxidative damage (e.g., G6PD deficiency)
- Polychromasia – Reflects increased circulating reticulocytes
In many cases, the smear provides the first clue to etiology before confirmatory testing.
Intravascular vs Extravascular Clues
- Intravascular hemolysis
- Hemoglobinemia
- Hemoglobinuria
- Markedly low haptoglobin
Extravascular hemolysis
- Splenomegaly
- Spherocytes on smear
- Mildly reduced haptoglobin
- These patterns help localize where destruction is occurring.
Additional Diagnostic Tests
To further define etiology:
- Direct Antiglobulin Test (DAT / Coombs test) – Autoimmune hemolysis
- G6PD assay – Enzyme deficiency (note: may be falsely normal during acute episodes)
- Hemoglobin electrophoresis – Hemoglobinopathies
- Osmotic fragility test – Hereditary spherocytosis
Laboratory Pitfalls
- Recent transfusion may mask hemolysis markers
- Liver disease can alter bilirubin interpretation
- Inflammation may falsely elevate haptoglobin
Always interpret results in clinical context.
Clinical Significance
Early recognition of hemolysis is critical for:
- Diagnosing autoimmune hemolytic anemia
- Detecting transfusion reactions
- Identifying inherited RBC disorders
Laboratory Takeaway
Hemolytic anemia is a pattern-based diagnosis.
No single test is sufficient – interpretation requires integrating:
- Biochemistry plus Hematology plus Morphology
Which marker do you find most reliable in early hemolysis – LDH, haptoglobin, or the peripheral smear?”
Stay updated with Hemostasis Today.
-
May 22, 2026, 17:30Veronica Sanchez: Do You Live with Pain after a Stroke?
-
May 22, 2026, 17:25Maxime Dely: A Simple but Powerful Indicator of Platelet Quality
-
May 22, 2026, 17:24Jim Hoffman: A New Approach to Balancing Host Defense and Tissue Protection
-
May 22, 2026, 17:22Lucia Rugeri: Advancing Multidisciplinary Care for Heavy Menstrual Bleeding in Women with Bleeding Disorders
-
May 22, 2026, 17:20Nour Al-Mozain: Optimizing PBSC Collection Through Real-Time CD34+ Monitoring
-
May 22, 2026, 16:30Buse Bor: New Publication on Therapeutic Interventions for Women with Obstetric APS
-
May 22, 2026, 16:29Danny Hsu: The Reversal Dilemma – Rethinking our approach to DOAC-associated ICH
-
May 22, 2026, 16:28Bartosz Hudzik: High Bleeding Risk Does Not Always Mean Bleeding-Risk Predominance
-
May 22, 2026, 16:26Sandeep De: Omicron COVID Infections Linked to Coronary Thrombosis without Detectable Plaque

