Yves Bikorimana: How a Simple Temperature Change Can Trigger Antibody-Mediated Destruction of RBCs
Yves Bikorimana, CEO at MedData – Rwanda and Lab Scientist at The University Teaching Hospital of Kigali – Chuk, shared a post on LinkedIn:
“Cold Agglutinin
1. Introduction
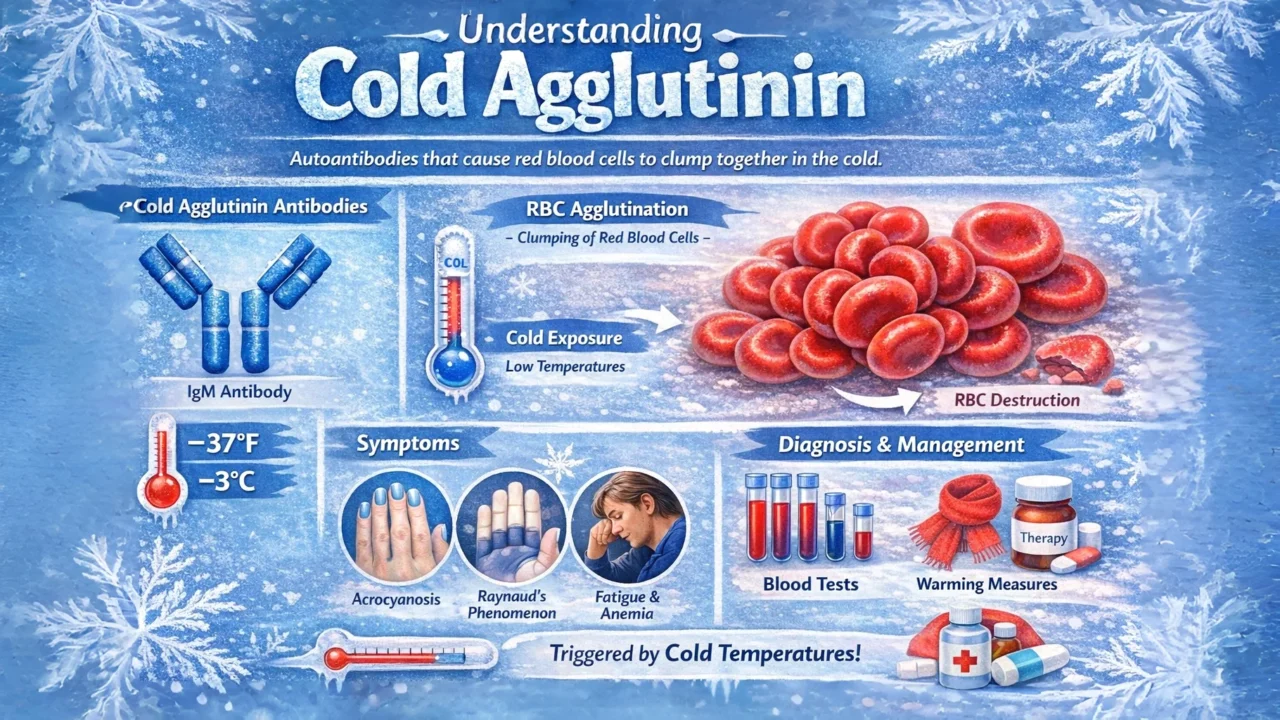
Cold agglutinins are autoantibodies (usually IgM) that bind to red blood cells (RBCs) when the body is exposed to cold temperatures.
When this happens, the red blood cells clump together (agglutinate) and may be destroyed, leading to a condition called Cold Agglutinin Disease (CAD), a type of autoimmune hemolytic anemia.
In simple words:
When the body gets cold, certain antibodies mistakenly attack red blood cells.
2. Clinical Significance
Cold agglutinins are important because they can cause:
- Acrocyanosis (bluish fingers, toes, ears)
- Symptoms worse in cold weather
- Fatigue
- Anemia
- Shortness of breath
- Jaundice (in severe hemolysis)
In laboratory practice, cold agglutinins can also:
- Interfere with blood grouping
- Affect complete blood count (CBC) results
- Cause false laboratory values if samples are not kept warm.
3. Physiopathology (What Happens in the Body)
Let’s break it down gently:
- In cold temperatures (usually below 30–32°C), IgM antibodies bind to RBC surface antigens (commonly the I antigen).
- This causes RBCs to clump together.
- The complement system gets activated.
- Red blood cells are destroyed (hemolysis), mainly in the liver.
- The patient develops anemia.
Key idea:
Cold – IgM binds RBC – Complement activation – Hemolysis – Anemia
4. Causes
Cold agglutinin production may occur due to:
Primary (Idiopathic)
- No clear underlying disease
- Often chronic
Secondary Causes
- Infections: such as Mycoplasma pneumoniae, Epstein-Barr virus (EBV),
- Lymphoproliferative disorders: Non-Hodgkin lymphoma, Chronic lymphocytic leukemia (CLL).
Autoimmune conditions:
It can be temporary (after infection) or chronic (especially in older adults).
5. How to Manage / Solve It
Management focuses on reducing symptoms and preventing hemolysis:
1. Avoid Cold Exposure
- Wear warm clothes
- Avoid cold drinks
- Keep IV fluids and blood warm
This is the most important step.
2. Treat the Underlying Cause
- Treat infection
- Manage lymphoma or autoimmune disease
3. Medical Treatment (in severe cases)
- Rituximab
- Immunotherapy
- Blood transfusion (with warmed blood if needed)
Note: Steroids are usually less effective compared to warm autoimmune hemolytic anemia.
Final Take-Home Message
Cold agglutinin disease reminds us how delicate the immune system is.
A simple temperature change can trigger antibody-mediated destruction of red blood cells.
Understanding it helps:
- Improve laboratory accuracy
- Prevent misdiagnosis
- Protect patients from complications”
Other posts featuring Yves Bikorimana on Hemostasis Today.
-
May 12, 2026, 16:46Tagreed Alkaltham: Why Apheresis Matters in Modern Transfusion Medicine
-
May 12, 2026, 16:37Reinhold Kreutz: Cardiovascular Burden in Acute Intermittent Porphyria Needs Greater Awareness
-
May 12, 2026, 16:33Pablo Corral: The Truth About Very Low LDL-Cholesterol
-
May 12, 2026, 16:24Mildred Lundgren: We Must Talk About the Invisible Causes of Stroke
-
May 12, 2026, 16:17Irene Scala: The Sex Disparities In Access to Acute Stroke Treatments In Italy
-
May 12, 2026, 16:04May Nour: UCLA Health Mobile Stroke Unit Becomes The 1st In The World to Perform mCTA In the Field
-
May 12, 2026, 15:57Leonardo Roever: Prognostic Impact of Lipoprotein(a) and CAR in Elderly Acute Ischemic Stroke Patients
-
May 12, 2026, 15:54Bruno Pougault: Prioritizing Laboratory Tests in Resource-Limited Emergency Care
-
May 12, 2026, 15:37Jennifer Holter Chakrabarty: Supporting the Next Generation of Hematology Researchers

