
Tareq Abadl: Persistent Anti-β2GPI IgG Is Not a Coincidence – It’s Pathology
Tareq Abadl, Medical Laboratory Specialist and Director of the Blood Bank at Dr. Abdelkader Al-Mutawakkil Hospital, shared a post on LinkedIn:
“β2 Glycoprotein I Antibodies — Made Simple
Many people hear the name β2 Glycoprotein I antibodies and get confused. Let’s break it down clearly
What is β2 Glycoprotein I?
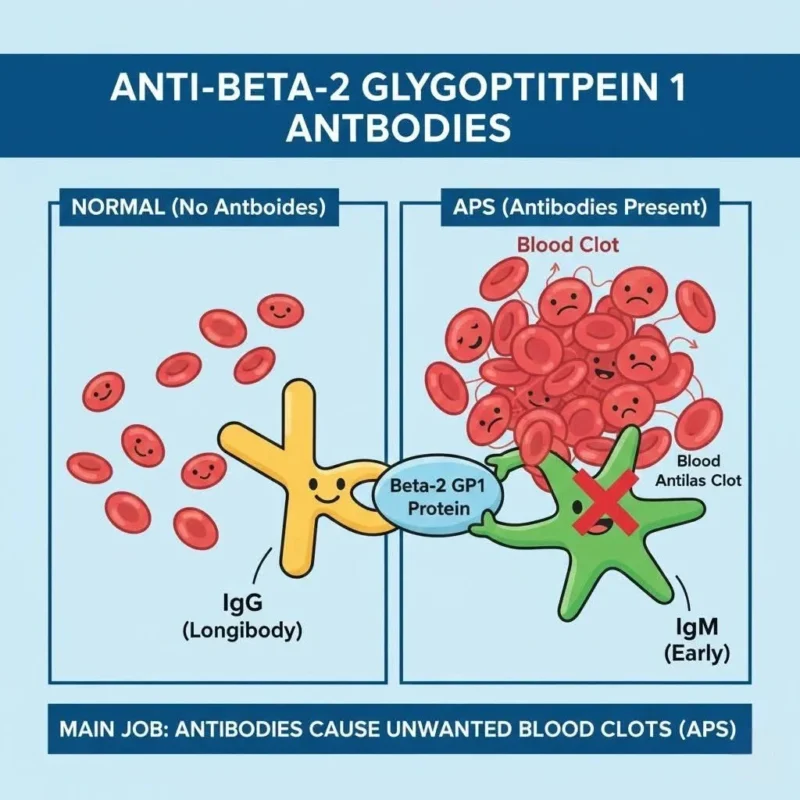
β2 Glycoprotein I (β2GPI) is a normal plasma protein that binds to phospholipids and plays a role in regulating coagulation.
What does the test measure?
It detects autoantibodies against β2GPI, which are a core laboratory criterion for diagnosing Antiphospholipid Syndrome (APS).
IgG vs IgM — What’s the difference?
β2GPI – IgM
- Often rises in early or transient immune responses
- May be associated with infections, inflammation, or immune stress
- Can be temporary and disappear on repeat testing
- Lower diagnostic weight for APS
β2GPI – IgG
- Clinically more significant
- Persistent elevation strongly supports APS diagnosis
- More clearly associated with:
- Thrombosis
- Recurrent pregnancy loss
- Placental insufficiency
Bottom line: IgG is more reliable and more dangerous than IgM in terms of complications.
Important Laboratory Points
The test must be repeated after ≥12 weeks to confirm persistence
- Never interpret it alone
- APS diagnosis requires a panel, including:
- Lupus Anticoagulant (LA)
- Anticardiolipin antibodies (aCL)
- Anti-β2 Glycoprotein I antibodies
- Medium to high titers are required — low positives may be clinically irrelevant
Advanced lab note (important):
- IgG antibodies targeting Domain I of β2GPI are the most pathogenic and most strongly linked to thrombosis
- Solid-phase assays (ELISA/CLIA) must follow international APS cut-offs, not manufacturer-only ranges
Simple analogy Anti-β2GPI antibodies are like someone sabotaging traffic control
Blood flow loses balance to congestion to clots
If IgG is present and persistent, this is not coincidence — it’s pathology.”
Find more posts featuring Tareq Abadl on Hemostasis Today.
-
May 12, 2026, 16:46Tagreed Alkaltham: Why Apheresis Matters in Modern Transfusion Medicine
-
May 12, 2026, 16:37Reinhold Kreutz: Cardiovascular Burden in Acute Intermittent Porphyria Needs Greater Awareness
-
May 12, 2026, 16:33Pablo Corral: The Truth About Very Low LDL-Cholesterol
-
May 12, 2026, 16:24Mildred Lundgren: We Must Talk About the Invisible Causes of Stroke
-
May 12, 2026, 16:17Irene Scala: The Sex Disparities In Access to Acute Stroke Treatments In Italy
-
May 12, 2026, 16:04May Nour: UCLA Health Mobile Stroke Unit Becomes The 1st In The World to Perform mCTA In the Field
-
May 12, 2026, 15:57Leonardo Roever: Prognostic Impact of Lipoprotein(a) and CAR in Elderly Acute Ischemic Stroke Patients
-
May 12, 2026, 15:54Bruno Pougault: Prioritizing Laboratory Tests in Resource-Limited Emergency Care
-
May 12, 2026, 15:37Jennifer Holter Chakrabarty: Supporting the Next Generation of Hematology Researchers

