
Islam Arid: Why We Say ‘Time is Brain’ when It’s Coming to Stroke Management?
Islam Arid, Registered Nurse at Memorial Hermann Health System, shared a post on LinkedIn:
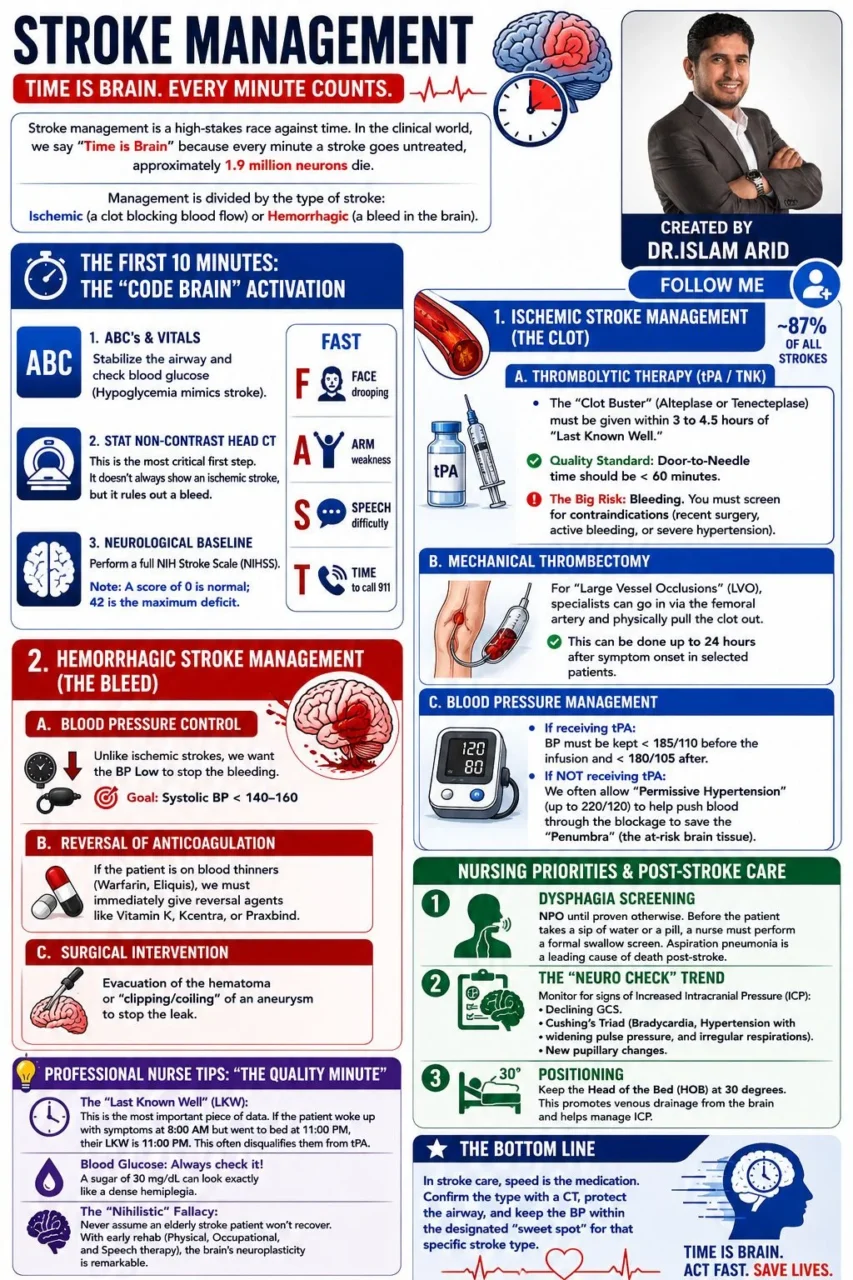
“Stroke management is a high-stakes race against time.
In the clinical world, we say ‘Time is Brain’ because every minute a stroke goes untreated, approximately 1.9 million neurons die.
Management is divided by the type of stroke: Ischemic (a clot blocking blood flow) or Hemorrhagic (a bleed in the brain).
The First 10 Minutes: The ‘Code Brain’ Activation
When a patient presents with stroke symptoms (FAST: Face drooping, Arm weakness, Speech difficulty, Time to call), the ‘Quality’ goal is a rapid, standardized assessment.
- ABC’s and Vitals: Stabilize the airway and check blood glucose (Hypoglycemia mimics stroke).
- Stat Non-Contrast Head CT: This is the most critical first step. It doesn’t always show an ischemic stroke, but it rules out a bleed.
- Neurological Baseline: Perform a full NIH Stroke Scale (NIHSS).
- Note: A score of 0 is normal; 42 is the maximum deficit.
1. Ischemic Stroke Management (The Clot)
About 87% of all strokes.
A. Thrombolytic Therapy (tPA / TNK)
The ‘Clot Buster’ (Alteplase or Tenecteplase) must be given within 3 to 4.5 hours of ‘Last Known Well.’
- Quality Standard: Door-to-Needle time should be < 60 minutes.
- The Big Risk: Bleeding. You must screen for contraindications (recent surgery, active bleeding, or severe hypertension).
B. Mechanical Thrombectomy
For ‘Large Vessel Occlusions’ (LVO), specialists can go in via the femoral artery and physically pull the clot out.
This can be done up to 24 hours after symptom onset in selected patients.
C. Blood Pressure Management
- If receiving tPA: BP must be kept < 185/110 before the infusion and < 180/105 after.
- If NOT receiving tPA: We often allow ‘Permissive Hypertension’ (up to 220/120) to help push blood through the blockage to save the ‘Penumbra’ (the at-risk brain tissue).
2. Hemorrhagic Stroke Management (The Bleed)
Caused by a ruptured aneurysm or uncontrolled hypertension.
A. Blood Pressure Control
Unlike ischemic strokes, we want the BP Low to stop the bleeding. The goal is typically a Systolic BP < 140–160.
B. Reversal of Anticoagulation
If the patient is on blood thinners (Warfarin, Eliquis), we must immediately give reversal agents like Vitamin K, Kcentra, or Praxbind.
C. Surgical Intervention
Evacuation of the hematoma or ‘clipping/coiling’ of an aneurysm to stop the leak.
Nursing Priorities and Post-Stroke Care
1. Dysphagia Screening
NPO until proven otherwise.
Before the patient takes a sip of water or a pill, a nurse must perform a formal swallow screen.
Aspiration pneumonia is a leading cause of death post-stroke.
2. The ‘Neuro Check’ Trend
Monitor for signs of Increased Intracranial Pressure (ICP):
- Declining GCS.
- Cushing’s Triad (Bradycardia, Hypertension with widening pulse pressure, and irregular respirations).
- New pupillary changes.
3. Positioning
Keep the Head of the Bed (HOB) at 30 degrees.
This promotes venous drainage from the brain and helps manage ICP.”
Stay updated with Hemostasis Today.
-
May 10, 2026, 15:14Could You Recognize Thrombotic Thrombocytopenic Purpura (TTP) in Time? – ASH
-
May 10, 2026, 15:13Deepak Lodha: PT and aPTT Mixing Study is a Key Tool in Coagulation Diagnosis
-
May 10, 2026, 15:12Marc Wittwer: Excellent Days at the 7th Coagulation Days in Zagreb
-
May 10, 2026, 15:12Tagreed Alkaltham: WB Donation vs Apheresis Donation – Understanding Donor Reactions and Why They Differ
-
May 10, 2026, 15:11Divyaswathi Citla Sridhar and Leonard Valentino Congratulate Roshni Kulkarni on Her Recognition as Advocate for Women and Girls with Bleeding Disorders
-
May 10, 2026, 15:09Haroun Gajraj: How Much of a Problem are Brown Marks after Sclerotherapy, Really?
-
May 10, 2026, 15:05Arun Chandran Nhattuvalappil: Simplifying Anticoagulation Decisions for Regional Anaesthesia with ASRA 2025 Guideline
-
May 10, 2026, 15:02Jean-Jacques Kiladjian: Inserm Grand Est Meeting on Clinical Research at CIC Strasbourg
-
May 10, 2026, 14:31Thomas Rocco: Humanity in the Age of AI

