
Ney Carter Borges: Contemporary Trends and Outcomes of Percutaneous Coronary Intervention for Stent Thrombosis
Ney Carter Borges, Member Cardiologist of Global Physician Association at Cleveland Clinic Florida, shared a post on LinkedIn:
”Contemporary Trends and Outcomes of Percutaneous Coronary Intervention for Stent Thrombosis
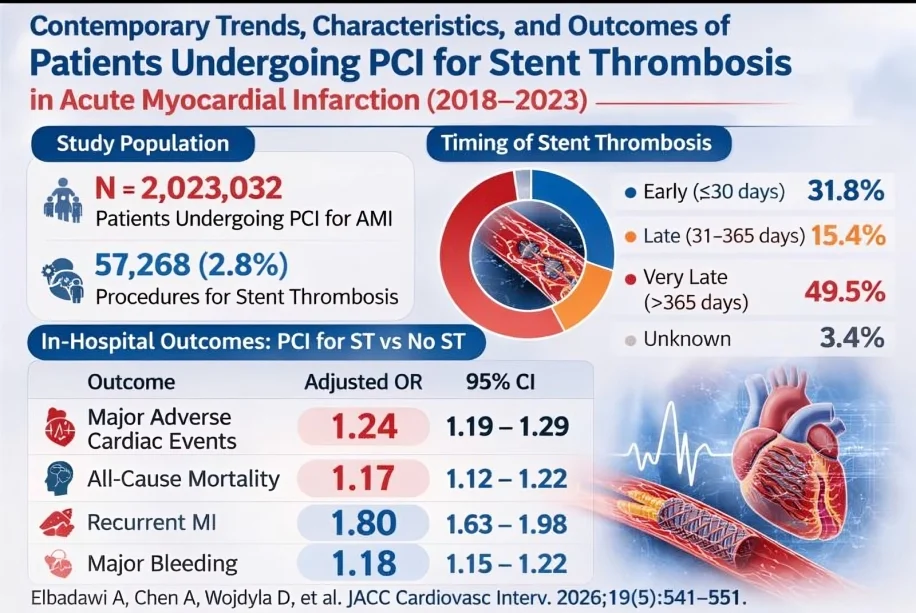
Stent thrombosis (ST) remains one of the most serious complications following percutaneous coronary intervention (PCI), frequently presenting as acute myocardial infarction (AMI). A contemporary analysis from the National Cardiovascular Data Registry (NCDR) CathPCI registry evaluated trends and outcomes of PCI performed for ST between April 2018 and June 2023. The study included 2,023,032 patients undergoing PCI for AMI, of whom 57,268 cases (2.8%) were attributed to stent thrombosis.
Regarding timing, very late ST (>365 days) represented the largest proportion of cases (49.5%), followed by early ST (≤30 days) at 31.8%, late ST (31–365 days) at 15.4%, and unknown timing in 3.4% of cases. Importantly, the incidence of PCI for ST remained stable over time, despite advances in contemporary PCI techniques, including newer-generation drug-eluting stents, potent P2Y12 inhibitors, and intracoronary imaging.
Clinically, patients with ST tended to be younger, more frequently male, and more likely to present with STEMI, cardiogenic shock, cardiac arrest, and ventricular arrhythmias, reflecting a high-risk population. Compared with PCI for non-ST lesions, PCI performed for ST was associated with significantly worse in-hospital outcomes, including higher rates of major adverse cardiac events (adjusted OR 1.24), all-cause mortality (OR 1.17), recurrent myocardial infarction (OR 1.80), and major bleeding (OR 1.18).
These findings highlight that, despite technological and pharmacologic advances, stent thrombosis remains a rare but high-risk complication of PCI, emphasizing the need for improved preventive strategies, optimized antithrombotic therapy, and procedural techniques to reduce its clinical impact.”
Other posts featuring Ney Carter Borges on Hemostasis Today.
-
May 12, 2026, 16:46Tagreed Alkaltham: Why Apheresis Matters in Modern Transfusion Medicine
-
May 12, 2026, 16:37Reinhold Kreutz: Cardiovascular Burden in Acute Intermittent Porphyria Needs Greater Awareness
-
May 12, 2026, 16:33Pablo Corral: The Truth About Very Low LDL-Cholesterol
-
May 12, 2026, 16:24Mildred Lundgren: We Must Talk About the Invisible Causes of Stroke
-
May 12, 2026, 16:17Irene Scala: The Sex Disparities In Access to Acute Stroke Treatments In Italy
-
May 12, 2026, 16:04May Nour: UCLA Health Mobile Stroke Unit Becomes The 1st In The World to Perform mCTA In the Field
-
May 12, 2026, 15:57Leonardo Roever: Prognostic Impact of Lipoprotein(a) and CAR in Elderly Acute Ischemic Stroke Patients
-
May 12, 2026, 15:54Bruno Pougault: Prioritizing Laboratory Tests in Resource-Limited Emergency Care
-
May 12, 2026, 15:37Jennifer Holter Chakrabarty: Supporting the Next Generation of Hematology Researchers

