
Ney Carter Borges: Sex Hormone Therapy and Thrombotic Risk – Balancing Benefits and Risks
Ney Carter Borges, Member Cardiologist of Global Physician Association at Cleveland Clinic Florida, shared a post on LinkedIn:
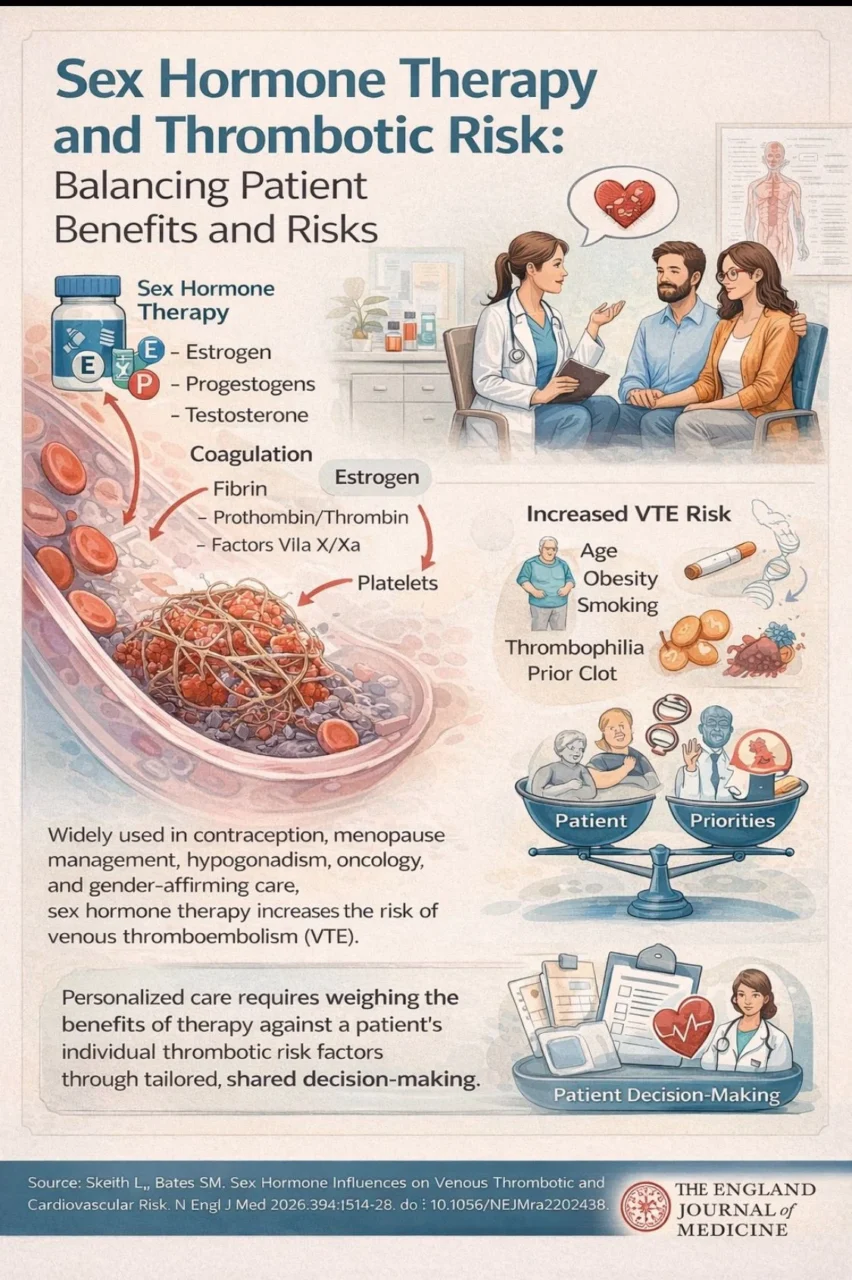
“Balancing Benefits and Risks: A Human-Centered View of Sex Hormone Therapy and Thrombotic Risk
Sex hormone therapy is deeply embedded in modern clinical care, supporting individuals across a wide spectrum of needs—from contraception and menopause management to gender-affirming treatment.
While its benefits are often substantial, its relationship with thrombotic and cardiovascular risk requires careful, individualized consideration.
At a biological level, estrogen plays a central role in increasing thrombotic tendency by shifting the hemostatic balance toward coagulation.
It enhances clotting factor activity while reducing natural anticoagulant pathways and promoting resistance to activated protein C.
Progestogens can amplify these effects depending on their formulation, whereas testosterone, when used at physiologic levels, appears to have minimal impact on coagulation, though supraphysiologic exposure may influence blood viscosity.
Clinically, combined oral contraceptives increase the relative risk of venous thromboembolism (VTE) approximately three- to fourfold, and hormone replacement therapy roughly doubles this risk.
However, translating these figures into real-world context is essential: in younger populations, the absolute risk remains low, which explains why these therapies are still widely considered safe for most individuals.
Importantly, not all formulations carry the same risk.
Lower estrogen doses and transdermal routes are associated with more favorable safety profiles, likely due to reduced hepatic effects.
Risk is not uniform.
Age, obesity, smoking, inherited thrombophilia, and prior thrombotic events significantly modify outcomes.
In such scenarios, decision-making becomes less about rigid rules and more about aligning medical evidence with patient priorities, tolerance for risk, and quality-of-life considerations.
In gender-affirming therapy, similar principles apply.
While the overall thrombotic risk is acceptable for most, avoiding higher-risk formulations such as ethinyl estradiol and favoring transdermal estradiol can meaningfully improve safety.
Ultimately, hormone therapy should not be viewed through a binary lens of ‘safe’ or ‘unsafe,’ but rather as a nuanced clinical tool.
When guided by evidence and shared decision-making, it allows clinicians and patients to navigate risk thoughtfully while preserving its meaningful therapeutic benefits.”
Other posts featuring Ney Carter Borges on Hemostasis Today.
-
May 12, 2026, 16:37Reinhold Kreutz: Cardiovascular Burden in Acute Intermittent Porphyria Needs Greater Awareness
-
May 12, 2026, 16:33Pablo Corral: The Truth About Very Low LDL-Cholesterol
-
May 12, 2026, 16:24Mildred Lundgren: We Must Talk About the Invisible Causes of Stroke
-
May 12, 2026, 16:17Irene Scala: The Sex Disparities In Access to Acute Stroke Treatments In Italy
-
May 12, 2026, 16:04May Nour: UCLA Health Mobile Stroke Unit Becomes The 1st In The World to Perform mCTA In the Field
-
May 12, 2026, 15:57Leonardo Roever: Prognostic Impact of Lipoprotein(a) and CAR in Elderly Acute Ischemic Stroke Patients
-
May 12, 2026, 15:54Bruno Pougault: Prioritizing Laboratory Tests in Resource-Limited Emergency Care
-
May 12, 2026, 15:37Jennifer Holter Chakrabarty: Supporting the Next Generation of Hematology Researchers
-
May 12, 2026, 15:21Joseph Mmwa: Blood Donation Debate Sparks Concern Across Kenya

