
Smitirupa Mishra: Early Clues Lie in Neutrophil Morphology
Smitirupa Mishra, Consultant Pathologist at Sparsh Hospitals and Lab Head at Pathkind Labs, shared a post on LinkedIn:
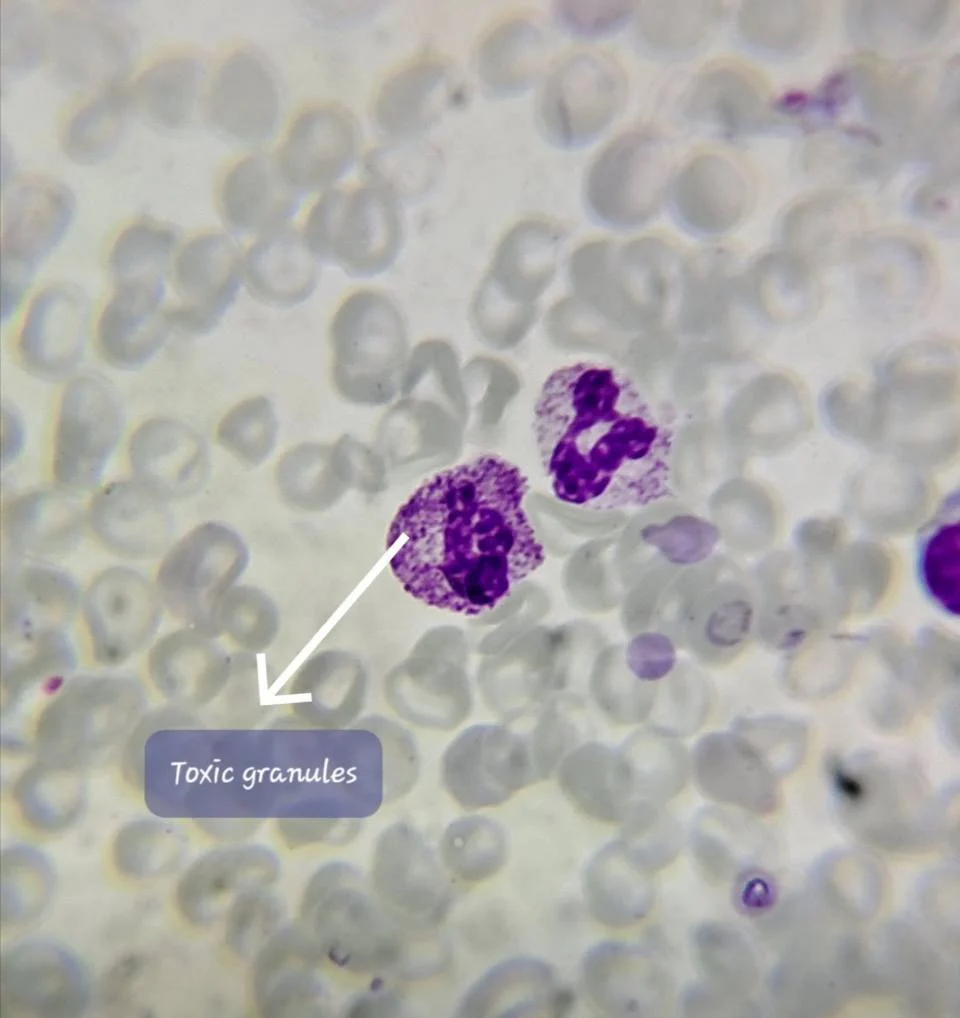
”Toxic Granules in Neutrophils – Practical Reporting and Clinical Relevance
Toxic granulation is not just a morphological curiosity-it is a dynamic indicator of systemic stress and marrow response, often guiding early clinical decisions.
What are Toxic Granules?
Coarse, dark blue-purple cytoplasmic granules in neutrophils representing retained primary (azurophilic) granules due to accelerated granulopoiesis under cytokine stimulation (e.g., IL-6, G-CSF).
How to Identify
Coarse, prominent, dark granules (larger than normal)
Uneven cytoplasmic distribution
Frequently associated with:
- Döhle bodies
- Cytoplasmic vacuolation
- Left shift
Always compare with internal control neutrophils on the same smear.
When Should You Report Toxic Granulation?
Based on Morphology (Primary Criterion)
Report when:
- Moderate to marked granulation
- Seen in a significant proportion of neutrophils
- Associated with other toxic changes
Should You Mention It with Normal or High WBC Counts?
Yes – WBC count does NOT limit reporting.
1. High WBC Count (Neutrophilia)
Most common scenario
Strongly supports acute bacterial infection / inflammation
Adds weight to a reactive process
2. Normal WBC Count
Very important to report
May indicate:
Early infection (before leukocytosis develops)
Localized infection
Immunocompromised states where WBC response is blunted
Toxic granulation can be an earlier and more sensitive marker than total leukocyte count.
3. Low WBC Count (Neutropenia)
If present, it is clinically significant and potentially alarming
Suggests:
Severe infection (e.g., sepsis) with marrow exhaustion
Clinical Significance
Seen in:
- Acute bacterial infections & sepsis
- Severe inflammation (burns, trauma)
- Post G-CSF therapy
- Pregnancy (mild)
What About Apoptotic Neutrophils?
How to Recognize Apoptotic Neutrophils?
Nuclear condensation (pyknosis)
Fragmentation (karyorrhexis)
Cytoplasmic shrinkage with or without vacuoles
Is there a correlation with toxic granulation?
- Toxic granulation indicates increased production and activation
- Apoptotic neutrophils indicate increased turnover and cell death
May indicate:
Intense inflammatory response with rapid neutrophil turnover
Seen in:
- Sepsis
- Severe infections
- Cytokine storm states
It reflects a high neutrophil kinetic state:
Increased production (toxic change) plus increased destruction (apoptosis)
How This Helps Clinicians
- Detect early infection, even with normal counts
- Identify severity and systemic involvement
- Distinguish reactive vs neoplastic neutrophilia
- Flag high-risk states (toxic changes plus neutropenia)
- Monitor treatment response
Pitfalls
- Don’t overcall in poorly stained smears
- Avoid reporting when minimal or focal
- Correlate with clinical context always
Take-Home Message
- Report toxic granulation based on morphology-not WBC count
- Its presence with normal or low counts is often more clinically significant
- Association with apoptotic neutrophils suggests high inflammatory turnover and severity.”
Stay updated with Hemostasis Today.
-
May 12, 2026, 16:37Reinhold Kreutz: Cardiovascular Burden in Acute Intermittent Porphyria Needs Greater Awareness
-
May 12, 2026, 16:33Pablo Corral: The Truth About Very Low LDL-Cholesterol
-
May 12, 2026, 16:24Mildred Lundgren: We Must Talk About the Invisible Causes of Stroke
-
May 12, 2026, 16:17Irene Scala: The Sex Disparities In Access to Acute Stroke Treatments In Italy
-
May 12, 2026, 16:04May Nour: UCLA Health Mobile Stroke Unit Becomes The 1st In The World to Perform mCTA In the Field
-
May 12, 2026, 15:57Leonardo Roever: Prognostic Impact of Lipoprotein(a) and CAR in Elderly Acute Ischemic Stroke Patients
-
May 12, 2026, 15:54Bruno Pougault: Prioritizing Laboratory Tests in Resource-Limited Emergency Care
-
May 12, 2026, 15:37Jennifer Holter Chakrabarty: Supporting the Next Generation of Hematology Researchers
-
May 12, 2026, 15:21Joseph Mmwa: Blood Donation Debate Sparks Concern Across Kenya

