
Tareq Abadl: Protective Role of Sickle Cell Trait in Malaria
Tareq Abadl, Medical Laboratory Specialist and Director of the Blood Bank at Dr. Abdelkader Al-Mutawakkil Hospital, shared a post on LinkedIn:
“Why Doesn’t Malaria Thrive in Some People?
The Secret of the ‘Sickle Cell Trait’
Nature sometimes protects humans in unexpected ways. One of the most fascinating examples is the relationship between malaria and the sickle cell trait.
The Problem: Plasmodium falciparum
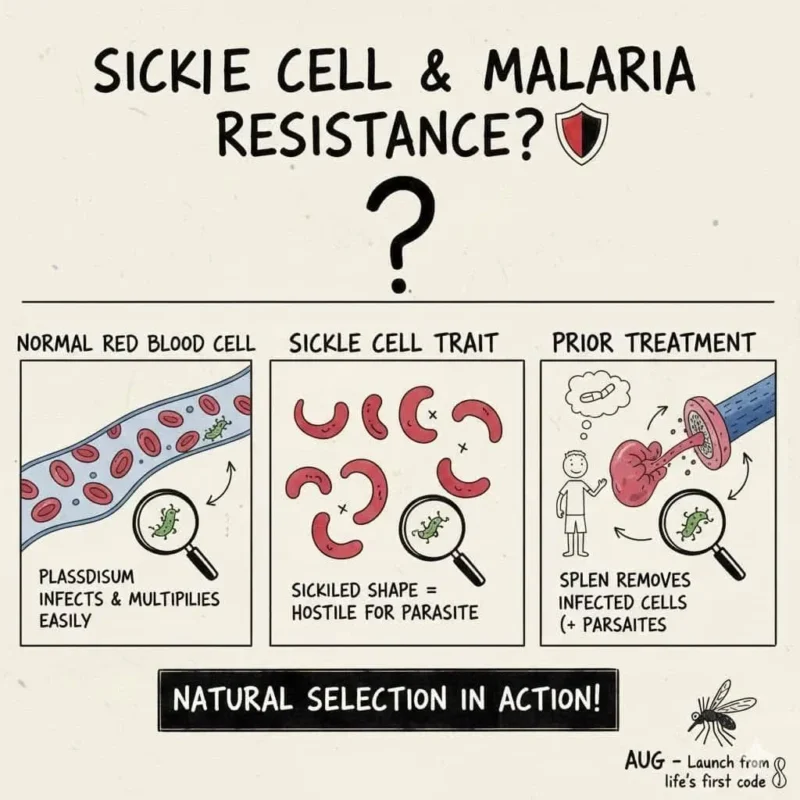
Malaria—especially the severe form caused by Plasmodium falciparum—invades red blood cells (RBCs), multiplies inside them, and eventually destroys them. This leads to anemia, organ damage, and potentially death.
The Genetic Twist: Sickle Cell Trait (HbAS)
People with sickle cell trait (HbAS) carry one normal hemoglobin gene (HbA) and one sickle gene (HbS).
Important clarification:
- Sickle Cell Disease (HbSS): serious inherited anemia
- Sickle Cell Trait (HbAS): usually healthy carriers with mild or no symptoms
The protective effect applies mainly to trait carriers (HbAS) — not those with full disease.
Why Malaria Struggles in HbAS Individuals?
Research shows several mechanisms:
- Reduced parasite growth
When P. falciparum infects HbAS red cells, low oxygen tension promotes mild sickling. These altered cells are less hospitable for parasite replication. - Enhanced removal by the spleen
Infected sickling RBCs are cleared faster by the spleen before the parasite can complete its life cycle. - Increased oxidative stress inside the cell
The altered hemoglobin environment creates oxidative conditions that impair parasite survival. - Reduced cytoadherence
Infected HbAS RBCs are less likely to stick to blood vessel walls, lowering the risk of severe malaria complications like cerebral malaria.
Classic Example of Natural Selection
In malaria-endemic regions (especially sub-Saharan Africa), the sickle cell gene became more common because:
HbAS individuals had better survival against severe malaria
They were more likely to reach reproductive age
The gene frequency increased over generations
This is called balanced polymorphism — where carrying one copy of a gene provides survival advantage.
Important Scientific Note
The trait does not provide complete immunity.
It mainly reduces the risk of severe and fatal malaria, particularly in childhood. Individuals can still become infected.
Newer Insights (Recent Research Trends)
Recent studies suggest:
- Protection may involve stronger innate immune activation
- HbAS may reduce expression of parasite proteins responsible for vascular adhesion
- There is growing interest in how this mechanism could inspire future malaria therapies
Bottom Line
Sickle cell trait is not a disease in most carriers — it’s a genetic adaptation shaped by evolutionary pressure from malaria.
One gene, one parasite, and millions of years of natural selection — a powerful story written in our red blood cells.”
Tareq Abadl, Malaria/LinkedIn
Find more posts featuring Tareq Abadl on Hemostasis Today.
-
May 29, 2026, 09:53Yassin Taher: Recognizing Clonal Eosinophilic Disorders in Pediatric Hypereosinophilic Syndrome
-
May 29, 2026, 09:52Sergio Emanuel Kaiser: Ruvonoflast and a New Anti-Inflammatory Strategy for Residual Cardiovascular Risk
-
May 29, 2026, 09:50Maria Symiakaki: Advancing Cardiovascular Prevention at the 2026 Congress of the European Atherosclerosis Society
-
May 29, 2026, 09:37Katie Baca-Motes: What Can Menstrual Cycle Physiology Tell Us About Health Beyond Reproduction?
-
May 29, 2026, 09:35Torben Boelk: Bringing Plasma Donation to the Heart of Leipzig
-
May 29, 2026, 04:37Josefin Ahnström: How Andexanet Alfa Impacts TFPIα Function
-
May 29, 2026, 03:19Building Safer Systems for Anticoagulation Management – ISTH
-
May 29, 2026, 03:07Early Diagnosis Can Change the Lives of Women With Haemophilia – EHC
-
May 29, 2026, 02:41Ifeanyichukwu Ifechidere: The Biggest DOAC Myth in Coagulation – ‘No Monitoring Required’

