
Dr Abdul Mannan on the Echinocyte: Mastering the Diagnostic Duality of Artifact vs. Pathology
Dr Abdul Mannan, Consultant Haematologist at Betsi Cadwaladr University Health Board, posted on LinkedIn:
“The Diagnostic Duality of the Echinocyte: Mastering the Artifact vs. Pathology Conundrum
Few findings are as deceptively simple—yet diagnostically complex—as the echinocyte.
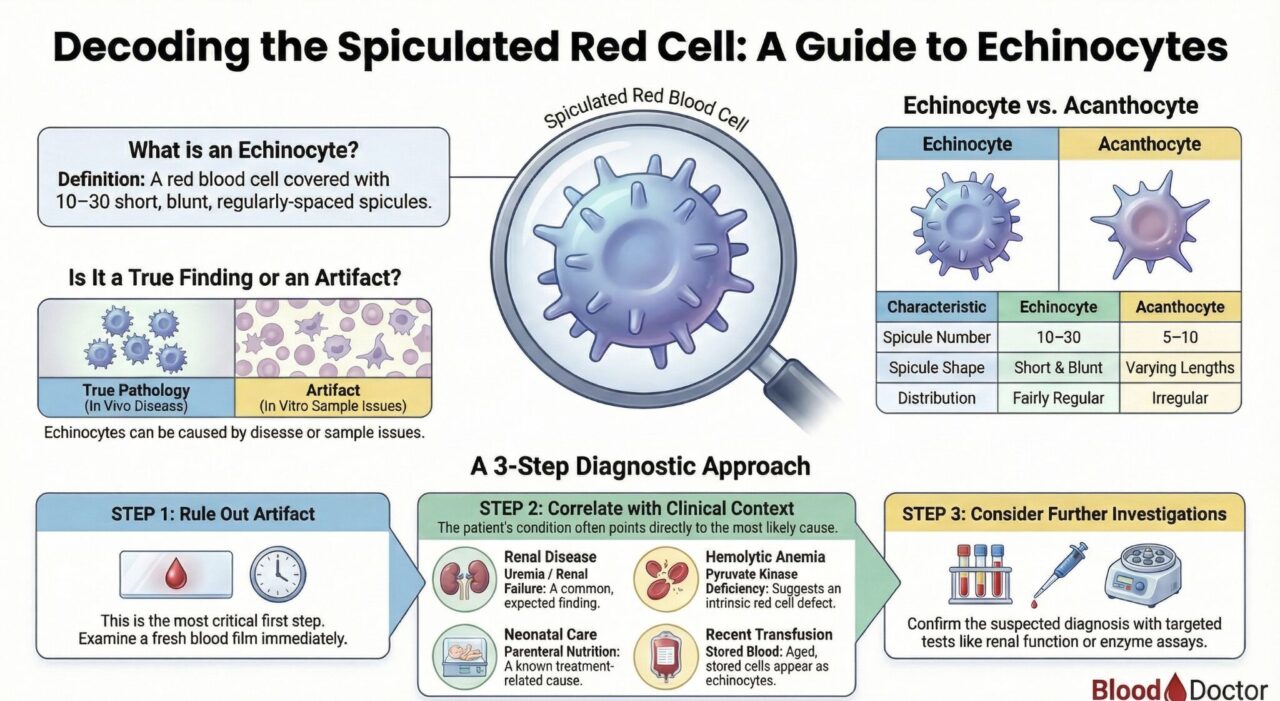
Often confused with the acanthocyte, the echinocyte is an erythrocyte defined by its 10–30 short, blunt spicules of fairly regular form.
However, the most crucial lesson in teaching echinocyte identification is not merely recognizing its shape, but understanding its diagnostic duality: Is this pathology, or is this an artifact?
An impressive hematologist knows that reporting ‘echinocytes present’ is only the beginning. The true value lies in systematically unlocking their meaning.
The Professional’s 3-Step Protocol for Echinocytes
When an automated alert or initial film suggests echinocytosis, the systematic approach immediately transforms a simple observation into a powerful diagnostic tool.
Step 1: Rule Out Artifact
The formation of echinocytes in vitro is remarkably common. Before considering systemic disease, you must exclude technical causes.
• Test for Time & Storage: Echinocytes are a common storage artifact if the blood sample (especially in EDTA) sits too long.
• Test for Contamination: Check for potential contamination (e.g., heparin), which can induce echinocyte formation.
• Confirm Persistence: Prepare a fresh wet preparation immediately. True in vivo echinocytes will persist; artifacts often disappear.
Step 2: Correlate with Clinical Context (Plasma vs. Cell Defect)
Once artifact is excluded, evaluate the clinical status against the known mechanisms:
1-Pathway Alteration of Plasma Environment (All cells affected)
Renal failure (uremia), Hyperthermia, Snake/Bee Venom
Renal failure (uremia), Hyperthermia, Snake/Bee Venom
2-Intrinsic Red Cell Abnormality (Only proportion affected)
ATP deficiency (e.g., Pyruvate Kinase deficiency)
Neonates, Patients with haemolytic anaemia
Step 3: Consider Targeted Investigations
The clinical context dictates the next action:
• If renal failure is suspected: Order Renal Function Tests
• If an enzyme defect is suspected: Order PK
• Review the history for Chlorpromazine or Parenteral Nutrition
The echinocyte is a fascinating morphological messenger. Its appearance requires us to move beyond basic pattern recognition and apply a rigorous, systematic, and clinically integrated approach. This discipline is what separates a technician from a hematology expert.”
Follow the latest with Hemostasis Today.
-
May 31, 2026, 12:55Rishiraj Sinha: Transfusion Evidence Library Round-Up – International Thalassaemia Day 2026
-
May 31, 2026, 12:40Tareq Abadl: Key Differences Between Immune Thrombocytopenic Purpura and Thrombotic Thrombocytopenic Purpura
-
May 31, 2026, 12:37Jeyaraj Pandian: World Stroke Organization Advances Stroke Education and Care in Central Asia
-
May 31, 2026, 12:31Stephen James Ryan: We Validated the Norwegian Version of the Vision Impairment Screening Assessment in Stroke
-
May 31, 2026, 12:01Sheila Cristina Ouriques Martins: We Provide Practical, Real-World Examples on How to Implement Stroke Prevention Strategies
-
May 31, 2026, 11:51Seema Dawood: Principles of Blood Smear Examination and Interpretation
-
May 31, 2026, 11:45Maria Cherska: Should We Continue Relying on Risk Prediction or Shift to Direct Detection of Atherosclerosis?
-
May 31, 2026, 11:34Jose Rubio: Advancing Lupus Care Through Community and Partnership
-
May 31, 2026, 11:23Eugene Fan: Advancing Peripheral Blood Film Analysis with Artificial Intelligence

