
Simon Senanu: Iron Deficiency Anemia vs Anemia of Chronic Disease
Simon Senanu, Medical Laboratory Scientist at Perkins Medical Centre, shared a post on LinkedIn:
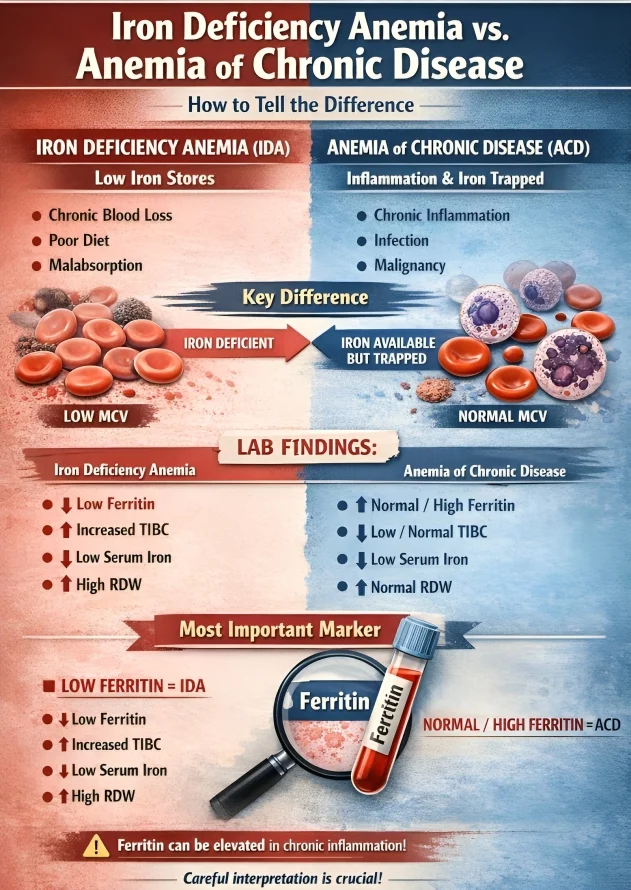
”Iron Deficiency Anemia vs Anemia of Chronic Disease – How to Tell the Difference
Microcytic or normocytic anemia is commonly encountered in clinical practice.
Two major causes are Iron Deficiency Anemia (IDA) and Anemia of Chronic Disease (ACD).
Although they may appear similar on a Complete Blood Count (CBC), their underlying mechanisms and laboratory patterns differ significantly.
Iron Deficiency Anemia (IDA)
IDA results from true depletion of iron stores, leading to reduced hemoglobin synthesis.
Common causes include:
- Chronic blood loss (e.g., menstruation, GI bleeding)
- Poor dietary intake
- Malabsorption
Anemia of Chronic Disease (ACD)
ACD also known as anemia of inflammation, occurs in the context of chronic immune activation.
Underlying conditions include:
- Chronic inflammation
- Infection
- Malignancy.
It is driven by hepcidin, which reduces iron availability by trapping iron in storage sites and decreasing intestinal absorption.
Key Pathophysiological Difference
In IDA, iron is deficient.
In ACD, iron is available but not accessible.
Laboratory Differences (How to Differentiate)
In Iron Deficiency Anemia:
- Hemoglobin is reduced
- MCV is typically low (microcytic)
- Serum iron is decreased
- Ferritin is low (reflecting depleted iron stores)
- Total Iron Binding Capacity (TIBC) is increased
- Transferrin saturation is reduced
- RDW is often elevated due to variation in RBC size
In Anemia of Chronic Disease:
- Hemoglobin is reduced
- MCV is usually normal or mildly decreased
- Serum iron is decreased
- Ferritin is normal or increased (iron is stored but unavailable)
- TIBC is low or normal
- Transferrin saturation is reduced
- RDW is usually normal or only slightly increased
Most Important Differentiator
Ferritin remains the single most useful marker
- Low ferritin strongly indicates IDA
- Normal or high ferritin suggests ACD, especially in inflammatory states
Diagnostic Pitfall
Ferritin is an acute phase reactant, meaning it increases during inflammation.
This can mask iron deficiency, making interpretation challenging in patients with chronic disease.
A patient with both iron deficiency and chronic inflammation may have a normal or elevated ferritin, masking IDA.
In such cases, additional tests become valuable:
- Soluble transferrin receptor (sTfR) – elevated in IDA, normal in ACD
- C-reactive protein (CRP) – helps assess inflammatory status
- sTfR/log ferritin index – improves diagnostic accuracy
Peripheral Smear Clues
Morphological examination can also provide supportive evidence:
- IDA: Microcytosis, hypochromia, anisopoikilocytosis
- ACD: Normocytic or mildly microcytic cells, less marked variation
Laboratory Takeaway
IDA and ACD may look similar on CBC, but iron studies, inflammatory markers, and clinical context reveal the difference.
Understanding this distinction is essential for accurate diagnosis and appropriate patient management.”
Other posts featuring Simon Senanu on Hemostasis Today.
-
May 12, 2026, 16:46Tagreed Alkaltham: Why Apheresis Matters in Modern Transfusion Medicine
-
May 12, 2026, 16:37Reinhold Kreutz: Cardiovascular Burden in Acute Intermittent Porphyria Needs Greater Awareness
-
May 12, 2026, 16:33Pablo Corral: The Truth About Very Low LDL-Cholesterol
-
May 12, 2026, 16:24Mildred Lundgren: We Must Talk About the Invisible Causes of Stroke
-
May 12, 2026, 16:17Irene Scala: The Sex Disparities In Access to Acute Stroke Treatments In Italy
-
May 12, 2026, 16:04May Nour: UCLA Health Mobile Stroke Unit Becomes The 1st In The World to Perform mCTA In the Field
-
May 12, 2026, 15:57Leonardo Roever: Prognostic Impact of Lipoprotein(a) and CAR in Elderly Acute Ischemic Stroke Patients
-
May 12, 2026, 15:54Bruno Pougault: Prioritizing Laboratory Tests in Resource-Limited Emergency Care
-
May 12, 2026, 15:37Jennifer Holter Chakrabarty: Supporting the Next Generation of Hematology Researchers

